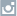TYPM does not encourage any illegal activities or the use or abuse of psychoactive plant medicine or psychedelics. Even within the confines of the law, they are not appropriate or beneficial for everyone.
Plant medicines and psychedelics are not “magical cures”, they are powerful tools, when used properly with respect, clear intentions, in a safe & supportive environment can catalyze personal growth and healing. They are not without serious risks.
In order to minimize harm and increase therapeutic potential, it is imperative to do your own research, prepare, and integrate your experience.
The material on this website is offered for informational use only, and is not intended for use in diagnosing or prescribing treatment for any disease or condition.
What is IBOGA?
Tabernanthe iboga is an evergreen rainforest shrub native to WestCentralAfrica. The bark and roots of the iboga plant contain high levels of the powerful psychoactive substance, ibogaine in addition to 11 other alkaloids (1). Other plants of the Apocynaceae family– such as the Tabernaemontanagenus – also contain Ibogaine.
The ibogashrubhas been and remains a central part of the Bwiti and Mbiri traditions of West-Central Africa for centuries. While lower doses are used to combat hunger and fatigue, and for their aphrodisiac effects, large doses are consumed in spiritual initiation rituals. With high doses, the iboga experience is marked by an intensity on emotional, visual, and physical levels and marked by visual introspection in a waking dream-like state (2). Iboga and its related alkaloids are not conducive to “recreational” experiences.
Iboga use in the West occurs for a variety of reasons ranging from its use as a stimulant, to treatment for substance use disorders through ibogaine-assisted therapy(there are approximately ninety clinics globally offering ibogaine treatment for addiction). There is also increasing interest in micro-dosing iboga to treat Parkinson’s Disease.
Recent reports suggest that the sustainability of Tabernanthe ibogaand related species may be in jeopardy due to over-harvesting and other environmental and social factors which threaten its natural habitat. The ramifications of these reports may threaten future availability of Iboga (3, 4 ).
Ibogaine, a psychoactive component of Iboga, has complex and poorly understood pharmacodynamics, targeting multiple neuro-transmittersincluding the kappa opioid, nicotinicand NMDA receptors. The potentialmedicalapplications of ibogaine treatment include neurological disorders, brain trauma and PTSD.(5).
Ibogaine is metabolized into noribogaine in the body. Noribogaine is long-lived and is thought to bind to and activate opioid receptors, which could be responsible for ibogaine’s potential analgesic and anti-addictive effects (6). Noribogaine, also acts to increase serotonin levels in the brain, which could also be responsible for its effects on mood, behavior, and depression (7).

READ MORE
Iboga is an established tradition in the Central West African spiritual practiceofBwiti, whichinclude the forest-dwelling Babongo, Mitsogo people of Gabon, and the Fang people of Gabon and Cameroon (8), where plants are revered and are referred to with terms such as “tradition”, “God”, and “knowledge” (9). Iboga, in particular, is a significant plant in Bwiti spiritual practices where it is used in high doses by initiates and more regularly in smaller doses in association with spiritual rituals. Although access to Bwiti traditions is limited, iboga is used by practitioners much like other traditional entheogenic plants, to induce feelings of insight and spiritual enlightenment. The experience of iboga consumption has been described as inducing a near-death experience that then leads to great spiritual understanding. Bwiti practice involves traditions including worship and connection with ancestors, animism, and ceremonies (10). The use of iboga may have played an important role in stopping the spread of Christianity and Islam in its native growing regions ( 11).
Iboga wasn’t discovered by the West until the late 19th century when European explorers reached Central West Africa and observed the use of iboga in traditional ceremonies. Ibogaine was isolated from the plant in 1901 but wasn’t properly synthesized until 1966.
Though both iboga, and its extract, ibogaine, hold therapeutic promise, the role of the accompanying role of the 11 alkaloids in the iboga plant(for example, ibogamine), though not currently understood, should not be discounted (12).
Iboga extractswereused mainly as a stimulant in the West until a heroin addict named Howard Lotsof consumed ibogaine(in 1962 in New York)and experienced a reduction in his heroin withdrawal symptoms. Lotsof’s friends also experienced similar anti-addictive effects and so with this anecdotal evidence, hesubsequentlycreateda pharmaceutical company to start clinical trials, and was awarded a patent in 1985 and 1992 for the ibogaine medication they developed as a treatment for acute addiction (13).
Ibogaine gained a reputation as a potential treatment for addiction and in 1993 the National Institute for Drug Abuse approved funding for stage 1 human trials, however, the death of a woman during treatment put the trial on hold (14).
Ibogaine is currently aSchedule 1 drug in the United States but has quasi-legalstatusin countries such as South Africa, Canadaand New Zealand.
While iboga’s roots lie in traditional African spiritual ceremonies, it and it’s related alkaloids hold much promise as a potential treatment for addiction and possibly depression, especially when combined with social support and a structured treatment plan (14).
Currently there are an estimated 100 ibogaine treatment facilities around the world.
Ibogaine, one of the alkaloids of iboga, demonstrably reduces the withdrawal symptoms of coming offopiates.It is also usedto reduce the withdrawal and addictive effects of cocaine, alcohol, and amphetamines. While the results are rapid and often extremely effective they are not are a cure-all for addiction and instead significantly reduce withdrawal symptoms for some time.
Addiction symptoms can be permanently stopped through ibogaine treatment but often return after weeks or months at reduced levels. Regardless of the variations in its effects, ibogainecan beeffective in treating addiction alongside psychotherapy.
- A review of 27 animal studies investigating the efficacy of ibogaine found that ibogaine treatment reduced self-administration of cocaine, alcohol, and opioids. This anti-addictive effect lasted for over 72 hours, with the more intense reduction in self-administration of substances seen in the first 24 hours following ibogaine administration (15).
- A study involving ibogaine as a treatment for opiate addiction showed both reduced self-reported opiate addiction symptoms and reduced physical signs of opiate withdrawal as determined by physicians (16).
- A long-term study of substance abuse symptoms studied30 patients receiving ibogaine treatment for their addiction issues. A baseline of drug frequency and dosage was measured before ibogaine treatment with patients being analyzed for addictive behavior every month for12 monthsfollowing treatment. The results showed that ibogaine’s anti-addiction effects showed the best results closest to the treatment. Only one-third of the study participants relapsed in the first month, while 60% relapsed by month two and 80% by month six (17).
- The safety and efficacy of ibogaine as a treatment for drug dependence was evaluated through a study of 75 previous addicts (alcohol,cannabis, cocaine, and crack-cocaine) who underwent a combined therapy of ibogaine treatment and psychotherapy. The study found no serious side effects or deaths from the combined therapy and impressively 61% of the study participants remained abstinent from their vices. Patients who received only one treatment of ibogaine remained abstinent for an average of five and a half months, while patients who received multiple ibogaine treatments remained abstinent for an average of just over eight months. Both the single and multiple ibogaine treatment results were statistically significant and lead to longer periods of abstinence than before ibogaine treatment. Ibogaine demonstrates a safe and effective treatment of addiction when used alongside psychotherapy (18).
While more research is needed into ibogaine’s potential antidepressant-like effects its effects on cognitive function and mood could play a role in reducing depression levels. Ibogaine therapymay help people who suffer from mood disorders view difficult experiences in an objective way, and may help facilitate the closure of unresolved emotional conflicts (19).
- The psychoactive effects of ibogaine could potentially treat depression and anxiety much like psychedelic-assisted therapy uses hallucinogens such as psilocybin (20).
- Current antidepressant drugs such as MAOIs and SSRIs have a significant binding affinity for sigma receptors, much like ibogaine does. This similar action on sigma receptors could indicate similar antidepressant effects in ibogaine as in SSRIs. SSRIs also work to improve depression by increasing serotonin levels, which ibogaine may also induce through sigma receptors (21).
It is critical to carefully consider your mindset, intentions, and safety and comfort of the environment before engaging in any activity that will expand your awareness, as this will profoundly affect the experience.
A common risk associated with iboga is the “bad trip” (anxiety, fear, paranoia). Iboga may provoke the onset of prolonged psychosis in vulnerable individuals making it critically important to investigate the mental history of family members before taking it, or any psychedelic.
“Because of the unregulated nature of ibogaine treatments, people are playing a lottery as to what kinds of results they will get,” says Hattie Wells of the Beckley Foundation. The quality of ibogaine treatment programs varies greatly. It is important to choose a reputable clinic withexperienced medical personnel, properscreening protocols,and apost-treatment support program (28). Integration and ongoing support from your community or mental health care professional plays an important role in therapeutic outcomes.
While ibogaine, holds much promise, especially as a treatment for addiction, the consumption of drugs such as heroin while taking ibogaine can have fatal consequences. Ibogaine is also unlike other psychedelics in that it is potentially cardiotoxic and physically dangerous. Side effects of iboga can include:
- Gastrointestinal issues
- Impaired muscle coordination
- Intense changes in visual and auditory perceptions
- Heart complications e.g. arrhythmia
Risk Of Death
It is very important to avoid using ibogaine if you have a pre-existing heart condition as this can cause adverse reactions and evenlead todeath (22).
One review identified 19 worldwide deaths attributed to ibogaine from 1990 to 2008 (23). These deaths were caused by several different factors including pre-existing heart issues, acute withdrawal from alcohol or benzodiazepines, and having one or more drugs co-administered with ibogaine (24).
The risk of death increases with a history of heart failure, childhood congenital heart defects, having an enlarged heart, history of stroke, irregular heart rhythms, and transient ischemic attacks. Iboga can also potentiate the effects of opiates and their lethality when co-administered. All substances must be given sufficient time to leave one’s system before ibogaine is administered with the half-life of all substances being carefully considered.
Ibogaine should always be administered under the supervision of a qualified medical professional to minimize potential adverse effects.
The Global Ibogaine Therapy Alliance has published a specific article outlining some of these points on iboga and death in more detail which you can read here.
Contraindications
With such serious side effects possible from ibogaine use, it’s important to be aware of any dangerous contraindications and avoid it if you have any.
Certain conditions are contraindicated because they pose a serious health risk. The following is an abbreviated list of these contraindicated condition, for a more detailed list visit Global Ibogaine Therapy Alliance. Consult your doctor before starting any ibogaine treatment.
- heart or heart-related conditions
- certain psychiatric conditions
- impaired liver or kidney function
- HIV treatment (risk of cardiac complications)
- gastric disorder, anti-fungal, or antihistamine medications – risk of cardiac complications
- Pregnant or breastfeeding women
- glaucoma or Alzheimer’s medication
- medication that is metabolized by the enzyme cytochrome P4502D6, meaning cardiac complications, and other dangerous effects are possible.
Read more about drugs that compete with Ibogaine and should be avoided by clicking here.
Addiction Potential
Ibogaine has a low potential for addiction and in fact, there is evidence ibogaine is itself an effective treatment for addiction. However, all psychedelics come with risks and you should only take ibogaine if prescribed by a doctor, especially if you’re taking ibogaine for healing from addiction. Certain withdrawal symptoms from substances such as opioids and alcohol can cause serious harm.
Long-Term Effects
The Multidisciplinary Association for Psychedelic Studies (MAPS) has completed two observational studies of ibogaine treatment’s long-term effects in Mexico and New Zealand (25,26). No evidence exists showing long-term adverse effects from single doses of ibogaine treatment as it’s commonly used for addiction treatment. In both studies, Ibogaine was well-tolerated and proved effective for decreasing drug dependence over 12 months.
Harm Reduction Measures
- Know why you are taking ibogaine
- Be aware of any pre-existing health conditions, and medications you’re taking that may negatively interact with ibogaine or any other risk factors that may affect you.
- Only take ibogaine with a trusted facilitator and under medical supervision, especially if undergoing addiction treatment.
- Use ibogaine in a safe and comfortable environment.
- Do not mix ibogaine with other drugs
- There is currently a shortage of iboga plants, it is wise to advocate for conservation measures, greenhouse growing, and sustainable practices (27), and to only use iboga when necessary.
For more harm reduction measures and additional information visit Global Ibogaine Therapy Allianceand the ICEERS Iboga page
Thank you to the Third Wave for generously allowing us to share their content. Visit the Third Wave for more information on Ibogaine
For more info on choosing a treatment center and preparing for the experience visit ICEERS
For additional info visit The Global Ibogaine Therapy Alliance and ICEERS